Hybrid Bone Marrow Aspirate,
The Best of Both Worlds!
Until recently, bone marrow aspirate was essentially always concentrated. However, there is now an ongoing debate between using bone marrow aspirate in a non-centrifuged manner and using it in a manner where it is concentrated by centrifugation. This question has generated much discussion and some heated debates in Regenerative Medicine circles. The question is, “Which group is correct?”
My answer is that both groups have valid points as to why theirs is the correct path to take. For this reason, we have come to the conclusion that a hybrid utilizing both centrifuged and non-centrifuged marrow aspirate works best, as has been borne out in our clinical results. Accordingly, for some time now, we have been performing what we call the Purbred-HybridTM technique.
The biggest argument in favor of centrifugation is that it will result in a greater concentration of stem cells from the bone marrow aspirate where the target cells are mesenchymal stem cells (MSC’s). There is little dispute over this fact and I agree with it one hundred percent. However, the real question to ask is whether MSC’s are the most important regenerative cell to enable success? There is no clear-cut answer to this question. What we can say is that we are becoming increasingly aware that a symphony of cells is needed for the greatest success. We need to move beyond early thinking that MSCs are the only important cells in marrow aspirate. MSC numbers may be an indication of good aspiration techniques but does this alone translate into good clinical success? Are we cutting off our nose to spite our face? In our quest to increase MSC numbers by centrifugation, are we sacrificing critical components of the marrow aspirate?
Some time ago I became aware that centrifuging bone marrow may also have drawbacks. In doing our research, one question we asked is whether or not any useful cells are being discarded in the centrifugation process. We felt that one such type of cell was the V-Cell [Very Small Embryonic-Like Stem Cell] whose characteristics are very similar to an early CD-133 stem cell. For more details, see the blog, Anti-Aging and Stem Cells.
On the positive side, there are other benefits of centrifugation beyond raising concentration. Stressing the cells, inherent in the process, can turn on certain metabolic switches driving the cells to repair and may well cause the production of a greater volume of growth factors. When all is said and done, growth factors are important contributors to success in regenerative procedures. The growth factors work in many different directions, including reducing local inflammation and, at the same time, encouraging repair.
Centrifugation also has a positive effect on MUSE BM stem cells. MUSE cells are pluripotent and can endure stressful situations such as those found in the joint. The stress of centrifugation may actually help the MUSE cell since they by and large thrive in stressful situations. On the negative side, centrifugation will probably remove some of the MUSE cells from the final product.
Another negative aspect is that centrifugation will change the shape of many cells and the number of cilia and thus the cell surface receptors. Therefore, I believe centrifugation will inevitably change the performance of both stem cells and other regenerative cells.
We also need to look at megakaryocytes and platelets. These cell types are what generate differentiation issues in bone marrow aspirate versus bone marrow concentrate. The bone marrow aspirate will contain more platelets so it will cause a different profile of cytokines. The cytokines from the platelets will cause the differentiation of cells to take on a different path, mainly hematopoietic differentiation. We know hematopoietic stem cells are one of the main drivers of tissue regeneration while mesenchymal stem cells are important for immune modulation.
The concentration of platelets may make a difference between centrifuged and non-centrifuged marrow aspirate. Fortunately, that difference can readily be equalized because platelets are easy to add. Indeed, for years, we have been adding PRP with every bone marrow injection.
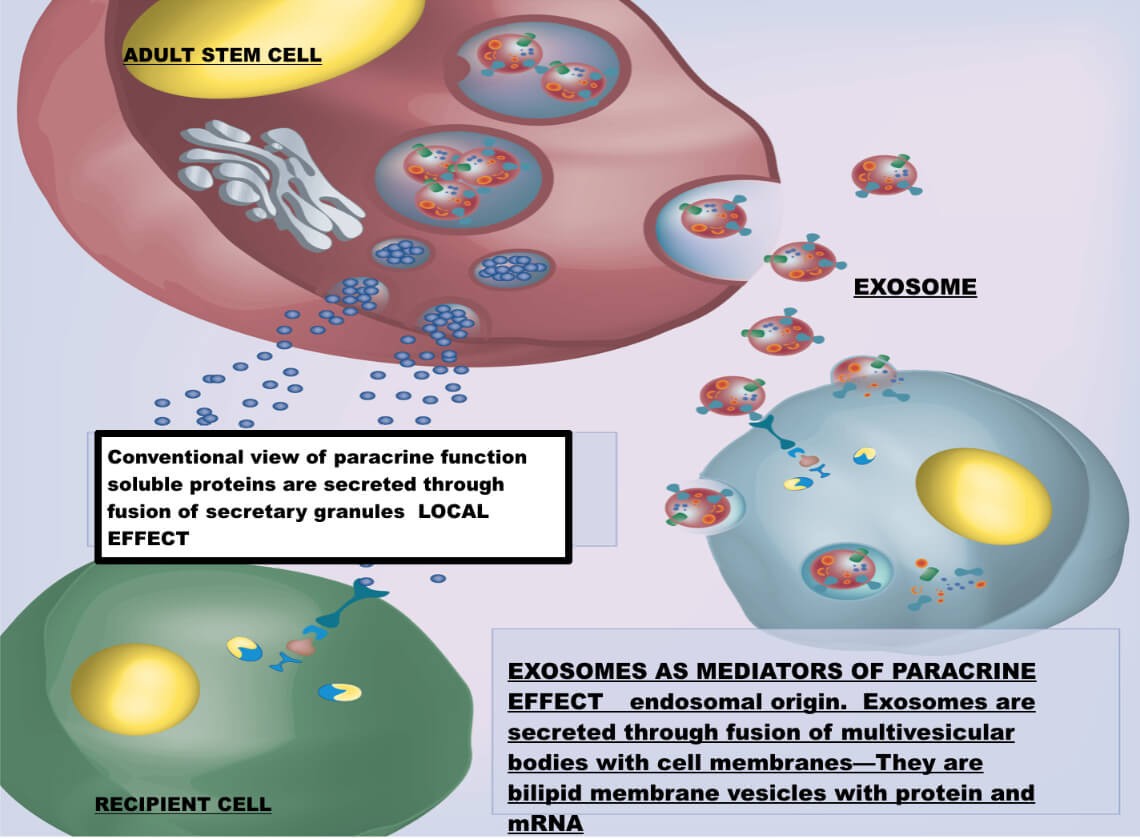
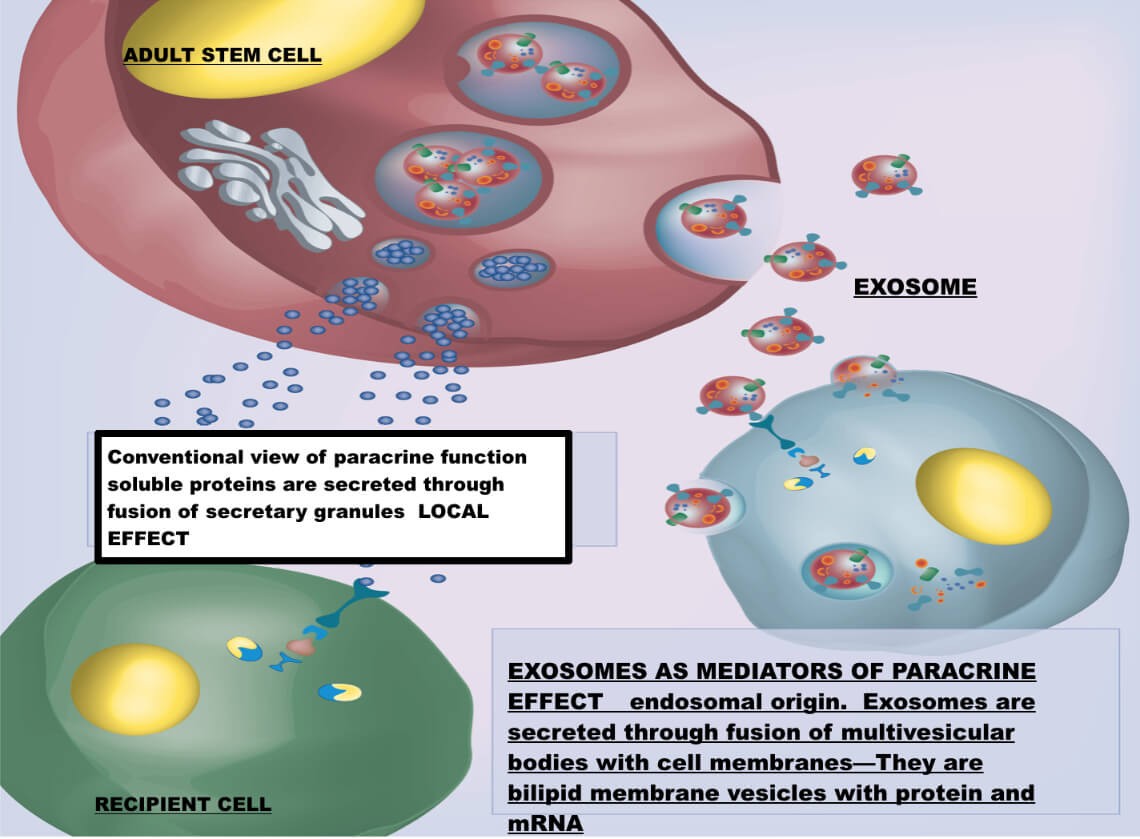
There are other components lost in the centrifugation processes that are not so easy to add. One such component is exosomes. Exosomes are much like the body’s Fed-Ex system in that they deliver growth factors to sites where they are needed. The exosomes contained in virgin aspirate may be more potent and more numerous than those found in centrifuged marrow. We must also realize exosomes may be a product of the cell environment. The various cells can sense what type of growth factors may be needed based on their environmental stimuli.
Neutrophils also play a huge role here in the two versions of bone marrow. Neutrophils basically control the oxygen uptake or “respiratory burst” that is so important to the viability of stem cells, especially vascular stromal cells. The respiratory burst does both good and bad. A respiratory burst will release free radicals (ROS) which can be bad for the overall environment of the regenerative cells (however, they are very good at killing pathogens). At the same time, the ROSs can have a profound effect on intracellular signaling pathways and ultimately in modulating gene expression. The following diagram shows the paradoxical effect of high levels of free radicals on cells. The opposite effect occurs in low levels of ROS.
Recent data have revealed that the respiratory burst is closely related to inflammation resolution in many instances. What else does the respiratory burst accomplish? Neutrophil respiratory burst-induced hypoxia activates macrophage erythropoietin signaling to promote acute inflammation resolution. This signaling is activated following inflammation.
Pharmacological or genetic inhibition of the respiratory burst suppresses hypoxia and macrophage erythropoietin signaling. An interesting experiment was performed in which a Macrophage-specific erythropoietin receptor-deficient mouse having chronic granulomatous disease (CGD) was utilized. These mice lacked the capacity for a respiratory burst, displayed impaired inflammation resolution and had symptoms of GCD. When given exogenous erythropoietin, it enhanced this resolution of the CGD.
How does centrifugation come into play here? Mechanical stress such as centrifugation causes major changes through reduced oxygen uptake especially in neutrophils. Centrifugation can negatively affect the “respiratory burst”. The reduced uptake of oxygen by the neutrophils caused by the mechanical stress of centrifugation will have a profound effect on transduction and differentiation and thus on the success of the bone marrow graft. There will be observable differences in the number of different cell types as well as in the downregulated pathways such as Macrophage 1 and Macrophage 2 conversion.
Macrophages have developed a unique ability to radically change their metabolism from a heal/growth promoting function, known as M-2, to an inhibit/kill function, known as M-1. This conversion is often dependent on the “neighborhood” in which the macrophage is found. This neighborhood is the extracellular matrix. The macrophages are the center of the immune “solar system”. Through these innate responses, macrophages are the central controlling element for tissue integrity and host defense while at the same time directing other cells of the immune system. The following diagram is a good example of this concept.
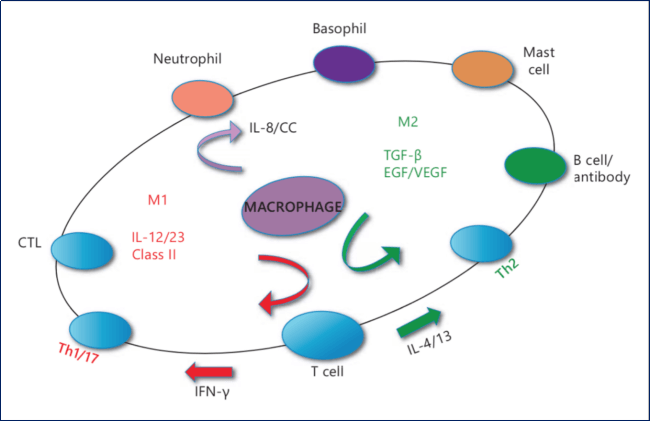
Macrophages – center of the immune solar system
We must ask the question, “Which of these cells are we discarding with centrifugation?” We must remember innate immune cells such as basophils and mast cells and other adaptive cells produce IL-4 and IL-13 priming M2 macrophage. IL-4 induced M2 macrophages expressed high concentration of IL-10, IL-1R antagonist, chemokines CCL22 and CCL17, and intracellular enzyme arginase-1.
All of these ensure the recruitment and activation of immune response and immune-suppressive function of M2 macrophages. In addition to immune response, IL-4 induced macrophages stimulate arginase activity by converting arginine to polyamines and collagen precursors that are crucial for tissue modeling and wound healing.
Macrophages were shown to be responsible for regeneration by actively metabolizing arginine with arginase into ornithine and urea. This is of upmost importance since macrophage production of ornithine is required for many repair processes because it is a precursor of the polyamines required for cell proliferation and collagen synthesis for extracellular matrix construction.
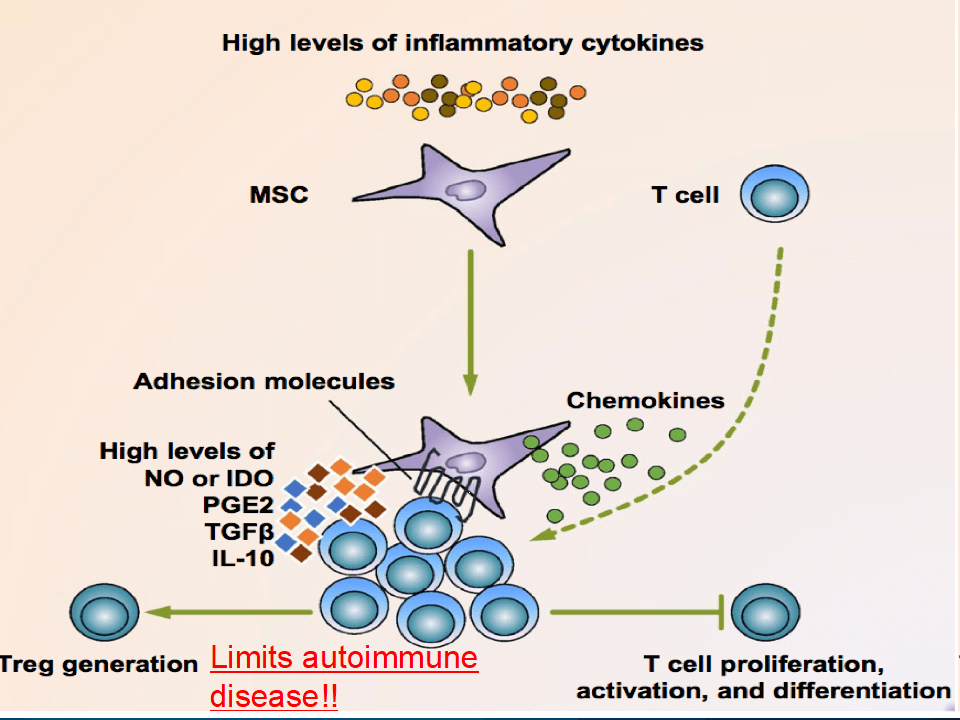
The M-1/M-2 conversion is of extreme importance. We now know that M-1/M-2 macrophage conversion can have a significant bearing on the ultimate success of a bone marrow graft. The following diagrams demonstrate this concept:
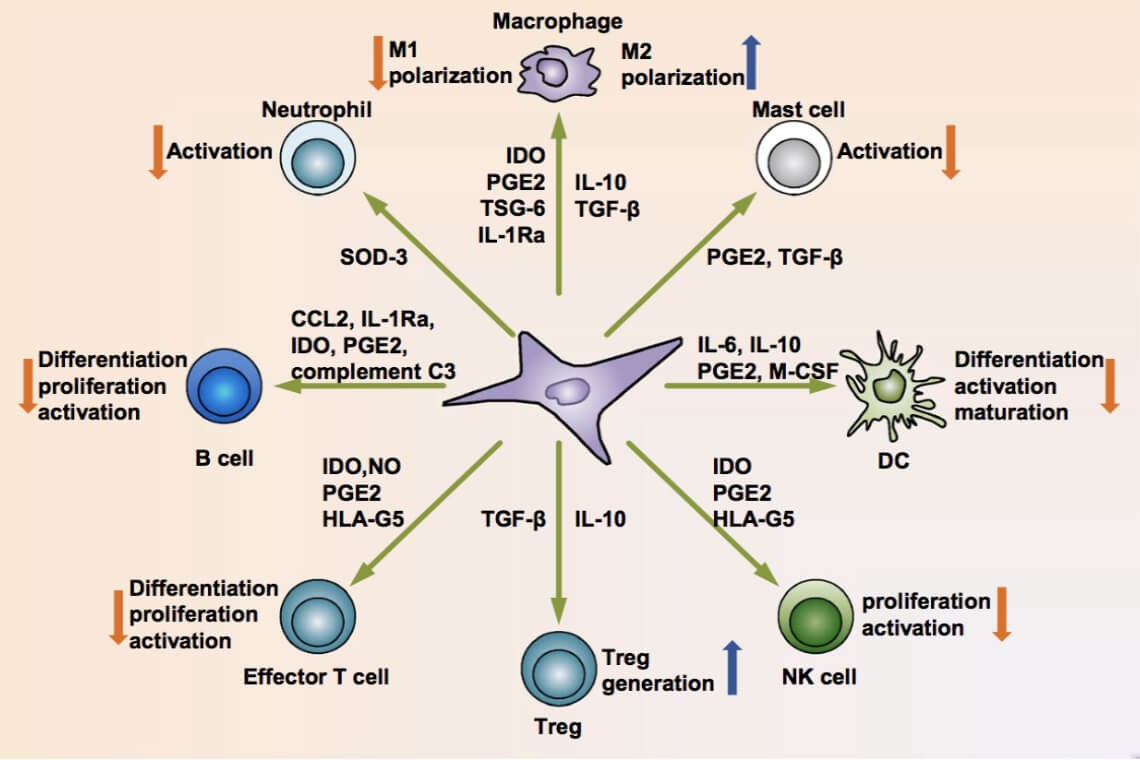


These diagrams show the relationship between the stem cells and the different types of macrophages. The environment in which macrophages are found determines what pathway they ultimately go down. Macrophages in M1 inhibit mode direct T cells to produce Th1-like cytokines (e.g. IFN-γ) that stimulate specific cytolytic T cells and activate more M1 macrophages. In contrast, macrophages in the M2/ heal mode stimulate T cells to produce Th2-like cytokines (e.g. IL-4 and TGF-β) that cause B cell proliferation and antibody production and further amplify M2 responses such as collagen precursors. Thus, macrophages actually use T cells as the ‘middle man’ to further amplify M1 or M2 dominant responses. In this case, the various cells of the immune system may be adversely affected by centrifugation. This can interfere with the M-1/M-2 conversion axis pushing it more towards the M-1 (inflammation) and away from M-2 (repair). This can have a profound effect on success of a bone marrow aspirate.
We can see that bone marrow aspirate is much more than just mesenchymal stem cells. It involves a symphony of cells from the immune system. We are now very much aware that MSCs alone are not the only immune modulator nor are they the only mediators cell repair. The cells of the immune system are very much involved in the success or failure of a regenerative medicine procedure. We need to realize that many different cells such as MSCs, HSCs, and the whole array of immune cells are important for regenerative success. Our techniques for marrow aspiration have improved and at the same time so has our final product. Over time, I have gone from full centrifugation to no centrifugation and now to our hybrid combining both techniques.
To quote one of my favorite Beatles songs, it’s been a “Long and Winding Road” to arrive at these conclusions. We can now see that both centrifugation and non-centrifugation have their merits and their drawbacks. Our results using a hybrid approach are clinically better. In our final hybrid product, the unspun marrow aspirate predominates in volume over the centrifuged marrow aspirate. However, more marrow aspirate is harvested for centrifugation than non-centrifugation.
I am also fortunate that in some of my clinics I have the ability to utilize a variety of cytokines such as IL-4 which helps regeneration by influencing macrophage polarization. As time goes on, I am sure that more refinements to the hybrid protocol will be made because this is an ever-changing field that constantly requires rethinking and re-evaluation.
Thanks, Dr. Purita
April 19, 2018
Source URL: https://stemcellorthopedic.com/hybrid-bone-marrow-aspirate-the-best-of-both-worlds/
